
There are three elements needed to establish service connection for PTSD in order to receive VA benefits. First, you must have a current diagnosis of PTSD from an expert who is competent to diagnose the disorder. Second, there must be credible supporting evidence that the claimed in-service stressor actually occurred. And third, there must be medical evidence of a causal nexus between the current symptomatology and the claimed in-service stressor. The following is a flow chart that you may use in order to determine what evidence is needed to establish service connection for a variety of situations.
In order for the VA to recognize a veteran’s PTSD in order to award service connection, the diagnosis must be provided by a qualified medical professional. Even though many veterans are treated by VA or private therapists who are not doctors or psychologists (i.e. licensed mental health social workers, licensed counselors, etc.), the VA will not accept their opinions initially diagnosing PTSD. According to the VA Clinician’s Guide (available to download on the VA website), professionals qualified to perform PTSD Compensation and Pension examinations (C&P exams) must have doctoral-level training in psychopathology, diagnostic methods, and clinical interview methods. They must have a working knowledge of the DSM-V and extensive clinical experience in diagnosing and treating veterans with PTSD. Persons with the requisite professional qualifications include board-certified psychiatrists and licensed psychologists, as well as psychiatric residents and psychology interns under the close supervision of an attending psychiatrist or psychologist.In addition, the diagnosis must conform to the diagnostic criteria in the DSM-V.
of the DSM-V and extensive clinical experience in diagnosing and treating veterans with PTSD. Persons with the requisite professional qualifications include board-certified psychiatrists and licensed psychologists, as well as psychiatric residents and psychology interns under the close supervision of an attending psychiatrist or psychologist.In addition, the diagnosis must conform to the diagnostic criteria in the DSM-V.
The most common reason the VA denies a claim for PTSD is because it believes that a veteran does not meet all of the diagnostic criteria in the DSM-V for PTSD. A veteran may be suffering from extreme PTSD, but if his or her symptoms do not fall neatly within the diagnostic criteria for PTSD, then for VA purposes, the veteran does not have PTSD, and service connection will be denied.
The diagnostic criteria in the DSM-V for PTSD are listed below (and may also be found on the VA website). After the stressor criterion, there are four symptom clusters: intrusion, avoidance, negative alterations in cognitions and mood, and alterations in arousal and reactivity. The sixth criterion concerns duration of symptoms, the seventh assesses functioning, and the eighth criterion clarifies that symptoms are not attributable to a substance or co-occurring medical condition. Note that some criterions require only one symptom, while others require multiple symptoms.
CRITERION A: STRESSOR
The person was exposed to: death, threatened death, actual or threatened serious injury, or actual or threatened sexual violence, as follows: (one required)
-
Direct exposure.
-
Witnessing, in person.
-
Indirectly, by learning that a close relative or close friend was exposed to trauma. If the event involved actual or threatened death, it must have been violent or accidental.
-
Repeated or extreme indirect exposure to aversive details of the event(s), usually in the course of professional duties (e.g., first responders, collecting body parts; professionals repeatedly exposed to details of child abuse). This does not include indirect non-professional exposure through electronic media, television, movies, or pictures.
Examples: Combat participation, military sexual trauma, witnessing a roadside bomb go off a few vehicles ahead, learning that a family member was killed in a car accident, or being part of a burial crew. Note that number three above may be the most difficult way to satisfy Criterion A. For instance, if the person involved is not a “close” friend, but the veteran made a decision that put that person in a dangerous situation and the person dies, this may not be enough to satisfy Criterion A even though the veteran may be traumatized because he or she feels responsible.
CRITERION B: INTRUSION SYMPTOMS
The traumatic event is persistently re-experienced in the following way(s): (one required)
-
Recurrent, involuntary, and intrusive memories.
-
Traumatic nightmares.
-
Dissociative reactions (e.g., flashbacks) which may occur on a continuum from brief episodes to complete loss of consciousness.
-
Intense or prolonged distress after exposure to traumatic reminders.
-
Marked physiologic reactivity after exposure to trauma-related stimuli.
CRITERION C: AVOIDANCE
Persistent effortful avoidance of distressing trauma-related stimuli after the event: (one required)
-
Trauma-related thoughts or feelings.
-
Trauma-related external reminders (e.g., people, places, conversations, activities, objects, or situations).
CRITERION D: NEGATIVE ALTERATIONS IN COGNITIONS AND MOOD
Negative alterations in cognitions and mood that began or worsened after the traumatic event: (two required)
-
Inability to recall key features of the traumatic event (usually dissociative amnesia; not due to head injury, alcohol, or drugs).
-
Persistent (and often distorted) negative beliefs and expectations about oneself or the world (e.g., “I am bad,” “The world is completely dangerous”).
-
Persistent distorted blame of self or others for causing the traumatic event or for resulting consequences.
-
Persistent negative trauma-related emotions (e.g., fear, horror, anger, guilt, or shame).
-
Markedly diminished interest in (pre-traumatic) significant activities.
-
Feeling alienated from others (e.g., detachment or estrangement).
-
Constricted affect: persistent inability to experience positive emotions.
CRITERION E: ALTERATIONS IN AROUSAL AND REACTIVITY
Trauma-related alterations in arousal and reactivity that began or worsened after the traumatic event: (two required)
-
Irritable or aggressive behavior
-
Self-destructive or reckless behavior
-
Hypervigilance
-
Exaggerated startle response
-
Problems in concentration
-
Sleep disturbance
CRITERION F: DURATION
Persistence of symptoms (in Criteria B, C, D, and E) for more than one month.
CRITERION G: FUNCTIONAL SIGNIFICANCE
Significant symptom-related distress or functional impairment (e.g., social, occupational).
CRITERION H: EXCLUSION
Disturbance is not due to medication, substance use, or other illness.
-
Specify if: With dissociative symptoms.
In addition to meeting criteria for diagnosis, an individual experiences high levels of either of the following in reaction to trauma-related stimuli:
-
Depersonalization: experience of being an outside observer of or detached from oneself (e.g., feeling as if “this is not happening to me” or one were in a dream).
-
Derealization: experience of unreality, distance, or distortion (e.g., “things are not real”).
-
Specify if: With delayed expression.



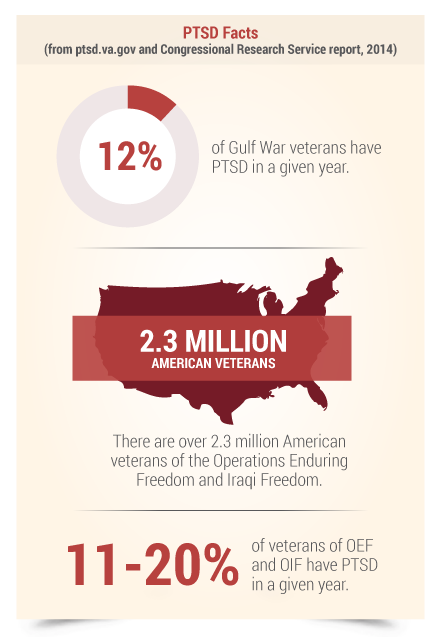
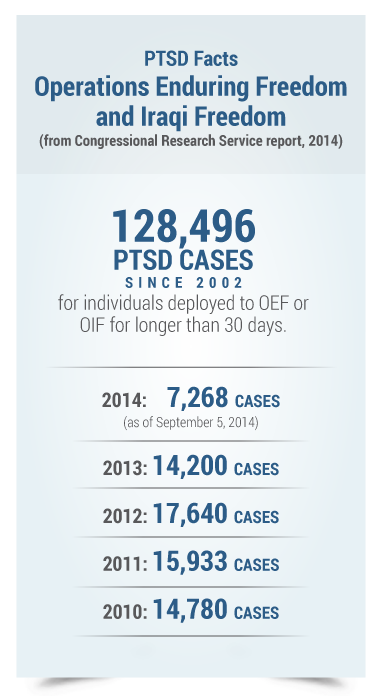
 The VA Adjudications Procedures Manual M21-1MR (available on the
The VA Adjudications Procedures Manual M21-1MR (available on the 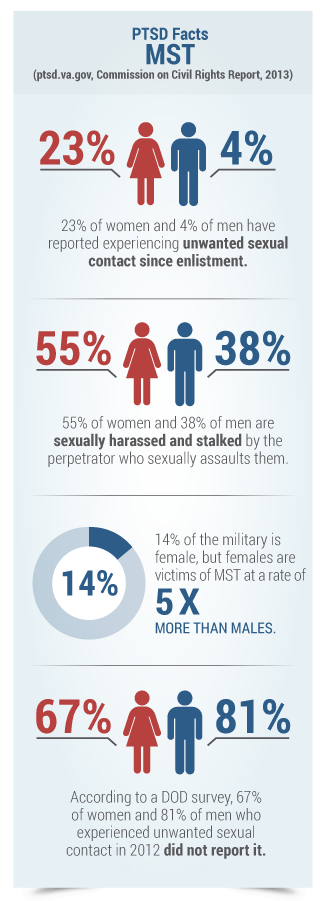
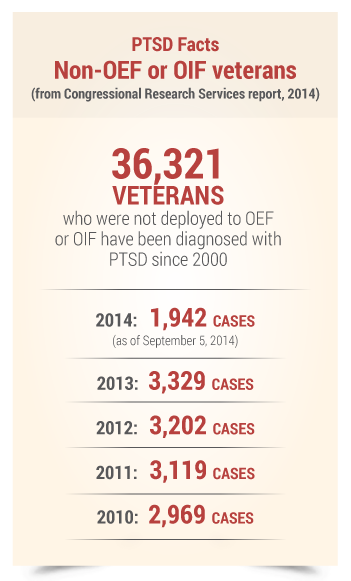 For the veteran’s service records to corroborate the stressor, they do not need to include every detail of the event. If there is independent evidence of the occurrence of a stressful event and that evidence shows the veteran’s personal exposure to the event, that could be sufficient corroborative evidence.
For the veteran’s service records to corroborate the stressor, they do not need to include every detail of the event. If there is independent evidence of the occurrence of a stressful event and that evidence shows the veteran’s personal exposure to the event, that could be sufficient corroborative evidence.

It is the service members who are undiagnosed are the ones I worry most about. Got to get help.
LikeLike